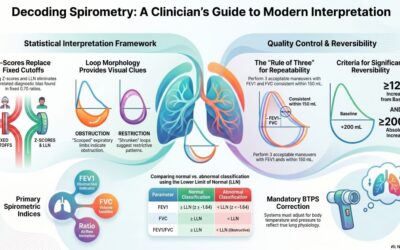
Modern spirometry systems measure dynamic airflow and lung volume parameters that directly reflect airway obstruction, reversibility, and disease progression in asthma and COPD. These systems capture forced expiratory volumes, flow–volume relationships, and reproducibility metrics that translate physiological impairment into actionable clinical data. Measurement precision supports differentiation between variable obstruction and fixed airflow limitation without relying on symptom reporting alone. Objective lung function data anchors diagnosis, staging, and monitoring decisions across care settings.
To clarify the clinical value of these measurements, modern systems consistently assess:
- Forced expiratory volume and capacity relationships
- Flow limitation across different lung volumes
- Effort consistency and maneuver repeatability
- Bronchodilator responsiveness patterns
- Longitudinal change across serial tests
Each data point contributes independently to diagnostic certainty and monitoring accuracy.
Why spirometry accuracy reshapes asthma diagnosis and classification
Accurate spirometry reshapes asthma diagnosis by confirming reversible airflow limitation rather than inferring disease from episodic symptoms. Modern systems reduce variability through automated quality checks that validate effort, timing, and repeatability. Improved accuracy prevents both overdiagnosis driven by transient symptoms and underdiagnosis masked by normal baseline exams. Reliable classification supports targeted therapy escalation without unnecessary exposure to long-term medications.
Accuracy improvements directly influence diagnostic outcomes by:
- Reducing false-positive asthma diagnoses
- Preventing symptom-driven misclassification
- Supporting objective confirmation of reversibility
- Enabling consistent reassessment over time
Precision at diagnosis establishes a stable foundation for long-term management.
Distinguishing intermittent from persistent airflow limitation
Spirometry differentiates intermittent obstruction from persistent impairment by comparing baseline and post-bronchodilator values across visits. This distinction prevents mislabeling episodic bronchospasm as chronic disease. Longitudinal tracking clarifies whether airflow limitation resolves or stabilizes over time.
How advanced spirometry improves early COPD detection
Early COPD detection improves when spirometry systems reliably identify subtle airflow decline before severe symptom onset. Modern sensors capture low-flow abnormalities and small airway changes that older devices often miss. Early identification supports earlier intervention, smoking cessation reinforcement, and risk stratification. Detection at earlier stages reduces diagnostic delay that accelerates functional decline.
Early-stage detection is strengthened through:
- Improved low-flow sensitivity
- Repeatable measurement across visits
- Trend visibility rather than single-test reliance
- Reduced dependence on patient-reported symptoms
Earlier detection shifts management from reactive to preventative.
Identifying preclinical airflow obstruction
Preclinical obstruction becomes visible when repeatable measurements reveal declining ratios despite minimal symptoms. Trend analysis highlights risk trajectories rather than isolated results. This approach supports proactive monitoring rather than delayed intervention.
Clinical value of real-time quality control during spirometry testing
Real-time quality control improves test validity by alerting clinicians to suboptimal effort, leaks, or timing errors during acquisition. Immediate feedback reduces repeat visits and unusable studies. High-quality data strengthens clinical confidence and minimizes interpretation ambiguity. Consistent test integrity supports comparability across visits and providers.
Quality control mechanisms commonly address:
- Inadequate expiratory effort
- Early termination of maneuvers
- Inconsistent start-of-test timing
- Leak detection during forced exhalation
- Failure to meet reproducibility thresholds
Each safeguard protects clinical interpretation from technical error.
Reducing technician-dependent variability
Automated prompts standardize coaching and acceptance criteria regardless of operator experience. Reduced variability improves reliability in busy outpatient and inpatient environments. Standardization protects clinical decisions from workflow pressures.
Why longitudinal lung function trending changes disease management
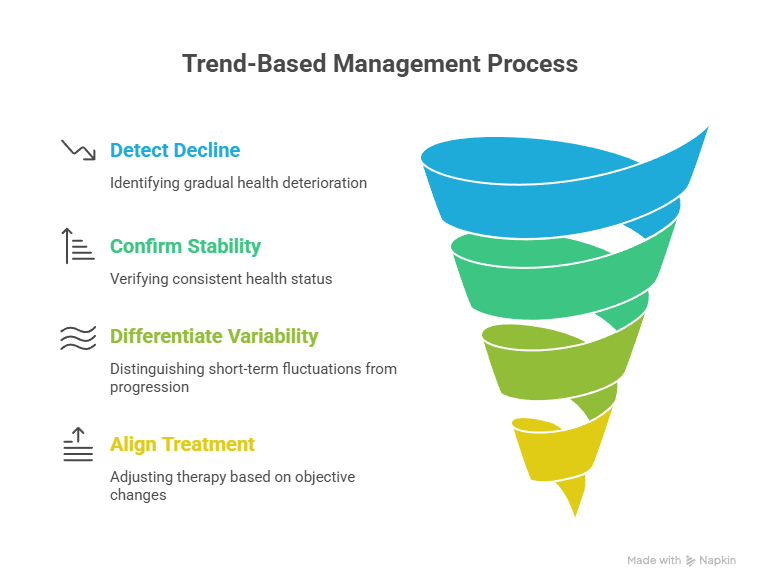
Longitudinal trending transforms spirometry from a diagnostic snapshot into a disease-management tool. Serial measurements reveal progression patterns that symptoms alone cannot capture. Trend visibility supports earlier therapeutic adjustments and validates treatment effectiveness. Continuous data strengthens shared decision-making between clinicians and patients.
Trend-based management enables clinicians to:
- Detect gradual decline before symptom escalation
- Confirm stability under maintenance therapy
- Differentiate progression from short-term variability
- Align treatment intensity with objective change
Longitudinal insight supports precision rather than episodic care.
Differentiating progression from variability
Modern systems separate natural variability from meaningful decline using consistent reference comparisons. This distinction prevents unnecessary escalation during transient fluctuations. Stable trends support treatment de-escalation when appropriate.
Operational impact of integrated spirometry data on clinical workflows
Integrated spirometry data improves efficiency by aligning testing, interpretation, and documentation within clinical workflows. Seamless data handling reduces transcription errors and report delays. Faster availability supports same-visit decision-making. Operational efficiency improves patient throughput without compromising diagnostic rigor.
Workflow integration commonly improves:
- Report availability timelines
- Documentation consistency
- Cross-provider data access
- Follow-up visit efficiency
- Care coordination across departments
Operational gains reinforce clinical quality rather than replacing it.
Supporting multidisciplinary respiratory care
Integrated reporting enables pulmonologists, primary care clinicians, and respiratory therapists to review consistent data. Shared access reduces interpretation discrepancies. Coordinated care improves continuity across settings.
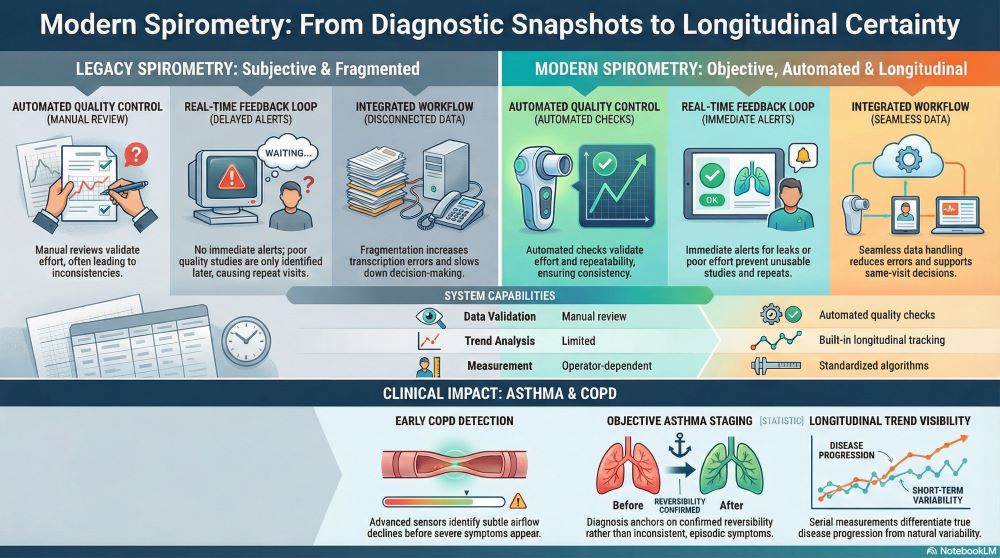
What differentiates modern spirometry from legacy systems in practice
Modern spirometry differs from legacy systems through enhanced sensors, automated validation, and data connectivity. Legacy devices often rely on manual interpretation and static outputs. Modern platforms prioritize repeatability, usability, and longitudinal insight. The practical result is higher diagnostic confidence with less operational friction.
The differences become clearer when viewed side by side:
| Capability | Legacy Spirometry | Modern Spirometry |
| Data validation | Manual review | Automated quality checks |
| Trend analysis | Limited | Built-in longitudinal tracking |
| Workflow integration | Standalone | Integrated reporting |
| Measurement consistency | Operator-dependent | Standardized algorithms |
| Clinical scalability | Limited | Designed for high-volume use |
These distinctions directly affect diagnostic reliability and follow-up quality.
Why standardized reference values matter for asthma and COPD assessment
Standardized reference values ensure lung function interpretation reflects population-appropriate norms. Modern systems incorporate updated reference frameworks that reduce misclassification across age, sex, and body size. Consistent benchmarks improve comparability between visits and facilities. Accurate referencing prevents inappropriate diagnosis driven by outdated norms.
Standardized references improve interpretation by:
- Reducing demographic bias
- Improving cross-site comparability
- Supporting consistent longitudinal assessment
- Aligning staging decisions across care teams
Reliable norms strengthen clinical confidence.
Minimizing demographic bias in interpretation
Updated reference alignment reduces bias in diverse patient populations. Objective normalization improves equity in diagnosis and staging. Precision supports fair clinical decision-making.
Clinical implications of reproducibility thresholds in spirometry
Reproducibility thresholds define whether spirometry results reflect true physiology or testing artifact. Modern systems enforce reproducibility automatically, preventing interpretation of unreliable data. Enforced thresholds protect against false trends. Reliable reproducibility underpins confident longitudinal assessment.
Reproducibility enforcement protects against:
- False improvement signals
- Missed disease progression
- Inconsistent follow-up decisions
- Misinterpretation due to poor effort
Reliable data integrity supports safer clinical decisions.
Preventing false reassurance or alarm
Poor reproducibility can mask deterioration or exaggerate improvement. Automated enforcement ensures only valid trends guide treatment. Clinical confidence improves when data quality is assured.
How spirometry supports personalized asthma management strategies
Spirometry supports personalization by objectively confirming control, reversibility, and response to therapy. Data-driven adjustment replaces symptom-based inference. Individualized plans improve adherence and outcomes. Objective measures strengthen trust between clinician and patient.
Personalization benefits include:
- Objective confirmation of treatment response
- Reduced reliance on subjective symptom reporting
- More confident therapy escalation or reduction
- Clear feedback for patient engagement
Objective data anchors individualized care.
Linking lung function to treatment response
Post-intervention spirometry verifies whether therapies improve airflow rather than symptoms alone. Measurable response supports continued therapy. Lack of improvement prompts reconsideration.
Role of spirometry in COPD phenotyping and risk stratification
Spirometry contributes to COPD phenotyping by quantifying severity and airflow limitation patterns. Objective staging informs prognosis and intervention intensity. Risk stratification supports appropriate resource allocation. Accurate phenotyping guides long-term management planning.
Spirometry-based phenotyping supports:
- Severity classification consistency
- Prognostic clarity
- Monitoring frequency decisions
- Escalation timing decisions
Structured phenotyping improves care planning.
Supporting stable versus exacerbation-prone classification
Serial spirometry identifies patients with accelerating decline. Early recognition supports intensified monitoring. Stable patterns justify maintenance strategies.
Why consistency across testing environments improves care continuity
Consistency across testing environments ensures spirometry results remain comparable across clinics and visits. Modern systems standardize measurement protocols. Continuity supports longitudinal interpretation despite care transitions. Reliable continuity reduces confusion and repeat testing.
Consistency benefits include:
- Reduced duplicate testing
- Clear comparison across care settings
- Improved discharge and follow-up alignment
- Stronger longitudinal insight
Standardization protects data integrity across transitions.
Managing inpatient to outpatient transitions
Standardized spirometry ensures inpatient assessments align with outpatient follow-up. Comparable data supports continuity of care. Transitional decisions become more reliable when lung function metrics remain consistent.
How modern spirometry systems support scalable respiratory programs
Modern spirometry systems support scalable respiratory care by balancing precision with operational efficiency. Standardized testing enables consistent expansion across clinics. Scalable systems maintain quality under higher patient volumes. Reliable scalability supports population-level respiratory management.
Programs benefit from scalability through:
- Consistent testing across locations
- Reduced training variability
- Centralized data interpretation
- Sustainable quality control
Scalability strengthens system-wide respiratory care.
Where spirometry system selection influences clinical confidence
Spirometry system selection influences clinical confidence by determining data reliability, interpretive clarity, and workflow fit. Systems that emphasize quality control and trend analysis reduce uncertainty. Confident interpretation supports decisive management. Reliable tools reinforce clinician trust in objective data.
Clinical confidence increases when systems provide:
- Clear quality validation indicators
- Consistent reproducibility enforcement
- Accessible longitudinal trends
- Intuitive reporting formats
System design directly impacts decision certainty.
Role of BOMImed in supporting modern spirometry integration
BOMImed supports modern spirometry integration by providing systems aligned with current clinical accuracy, reproducibility, and workflow expectations. Access to contemporary spirometry platforms enables clinicians to maintain diagnostic consistency while supporting longitudinal disease management. Alignment between equipment capability and clinical need reinforces reliable asthma and COPD assessment. Practical integration supports both individual patient care and broader respiratory programs.
Frequently Asked Questions
What does spirometry show for asthma management?
Spirometry shows whether airflow limitation is present and whether it improves with bronchodilator therapy, supporting objective confirmation of asthma control and reversibility.
How often should spirometry be performed in COPD patients?
Spirometry is commonly performed at diagnosis and periodically thereafter to monitor progression, treatment response, and stability.
Can spirometry detect COPD before symptoms appear?
Spirometry can reveal airflow limitation before significant symptoms develop, supporting earlier identification and monitoring of at-risk individuals.
Why is reproducibility important in spirometry testing?
Reproducibility ensures that measured changes reflect true lung function rather than testing variability or poor effort.
Does spirometry replace symptom assessment?
Spirometry complements symptom assessment by providing objective lung function data that symptoms alone cannot reliably indicate.
What makes modern spirometry more reliable than older devices?
Modern systems improve reliability through automated quality control, standardized interpretation, and longitudinal trend tracking.
Can spirometry results vary between clinics?
Standardized modern systems reduce inter-clinic variability, improving comparability across care settings.
Here’s a soft, professional CTA you can place at the bottom of the article. It’s informational-first, low pressure, and aligned with medical decision-makers who want clarity before engaging.
Learn More About Modern Spirometry Solutions
If you’re evaluating spirometry systems or need deeper insight into how modern pulmonary diagnostics can support obstructive lung disease assessment, BOMImed is available to help.
Our team works closely with clinics, hospitals, and healthcare professionals to provide clear guidance on spirometry technology, system capabilities, and clinical applications—without unnecessary complexity.
For additional information or to discuss your specific needs:
- Contact Page: https://bomimed.ca/contact/
- Phone: 1-866-830-4592
- Email: info@bomimed.ca
Whether you’re comparing systems, planning an upgrade, or looking for expert input, we’re happy to support your decision-making process.