Modern Spirometry Data Interpretation: ATS/ERS Standards, Z-Scores, and the Lower Limit of Normal
Modern spirometry output is far more than a set of raw numbers. Understanding how ATS/ERS technical standards, statistical reference models, flow-volume loop morphology, and quality grading work together is essential for accurate pulmonary function assessment — whether in a hospital-based lab or a Canadian primary care setting.
ATS/ERS Standards Govern Modern Spirometry Output
Modern spirometry output is a standardized dataset combining high-resolution airflow measurements, derived pulmonary indices, and statistically normalized reference comparisons. The framework governing this output comes from the joint technical standards published by the American Thoracic Society (ATS) and European Respiratory Society (ERS).
These standards define signal acquisition requirements, acceptability criteria, repeatability thresholds, and reporting formats to ensure consistency across devices and clinical environments. Properly structured output includes raw measurements, predicted values, z-scores, and the lower limit of normal (LLN) — enabling statistically valid interpretation rather than reliance on arbitrary thresholds.
The shift toward distribution-based interpretation reflects the adoption of global reference equations, including multi-ethnic datasets, which improve diagnostic accuracy across diverse populations — including those seen in Canadian clinical settings.
Primary Spirometric Parameters: What Each Index Measures
Spirometry measures airflow and volume relationships during forced respiratory maneuvers, capturing the interaction between airway resistance, lung compliance, and expiratory effort. All primary indices are derived from a forced expiratory maneuver initiated at total lung capacity and sustained until residual volume or a defined plateau is reached.
| Parameter | Definition | Primary Clinical Use |
|---|---|---|
| FEV1 | Volume exhaled in the first second of a forced maneuver | Sensitive indicator of airway obstruction |
| FVC | Total volume exhaled during a full forced maneuver | Baseline for ratio calculations; reduced in restriction |
| FEV1/FVC Ratio | FEV1 expressed as a proportion of FVC | Identifies airflow limitation independent of lung size |
| PEF | Maximum instantaneous expiratory flow rate | Effort-dependent; useful for monitoring, not diagnosis alone |
| FEF25–75 | Mean flow rate during the middle 50% of the FVC maneuver | Reflects small airway contribution; limited standalone specificity |
All derived indices must be interpreted within the context of statistical reference values, as raw measurements do not account for demographic variability.
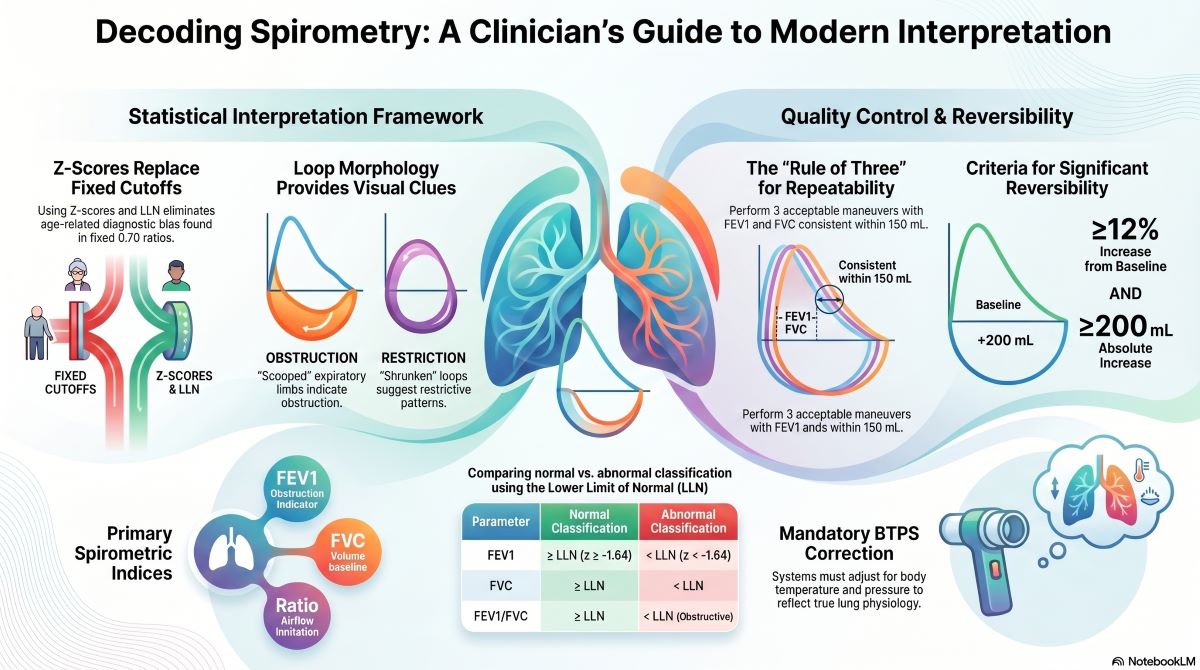
Lower Limit of Normal and Z-Score Interpretation Eliminate Age-Related Diagnostic Bias
The Lower Limit of Normal (LLN) and z-scores provide a statistically valid framework for interpreting spirometry results based on population distributions. The LLN represents the fifth percentile of a reference population and corresponds to a z-score of approximately −1.64. Values below this threshold indicate abnormality with defined statistical confidence.
Why Fixed Cutoffs Are Insufficient
Fixed thresholds — most commonly FEV1/FVC < 0.70 — introduce systematic misclassification:
- Overdiagnosis in older adults due to physiologic age-related decline in FEV1/FVC
- Underdiagnosis in younger patients whose ratios remain above 0.70 even with early disease
- Inconsistent interpretation across demographic groups not represented in the threshold's origin population
Z-score–based interpretation accounts for age, sex, height, and ethnicity, ensuring that measured deviations reflect true physiological abnormality rather than expected variation.
Parameter Interpretation Framework
| Parameter | Normal Classification | Abnormal Classification |
|---|---|---|
| FEV1 | ≥ LLN (z ≥ −1.64) | < LLN (z < −1.64) |
| FVC | ≥ LLN | < LLN |
| FEV1/FVC | ≥ LLN | < LLN → Obstructive pattern |
Canadian pulmonary practice increasingly aligns with these statistical models, particularly in hospital-based and diagnostic laboratory environments where multi-ethnic patient populations require accurate classification across demographic groups.
Flow-Volume Loop Morphology Provides Diagnostic Signal Beyond Numeric Indices
Flow-volume loops encode the mechanical behavior of the respiratory system and reveal abnormalities that scalar measurements cannot capture. The expiratory limb reflects airflow limitation during exhalation, while the inspiratory limb provides insight into upper airway function. Curve morphology must be evaluated alongside numeric indices to identify patterns and technical artifacts.
Diagnostic Patterns Identifiable on Flow-Volume Loops
| Pattern | Morphology | Clinical Implication |
|---|---|---|
| Obstructive | Concave ("scooped") expiratory limb with reduced PEF | Airway obstruction (asthma, COPD) |
| Restrictive | Reduced total volume; preserved contour and proportional flow | Parenchymal or chest wall restriction |
| Variable extrathoracic obstruction | Flattened inspiratory limb | Upper airway lesion (vocal cord dysfunction, tracheal stenosis) |
| Variable intrathoracic obstruction | Flattened expiratory limb | Intrathoracic tracheal or large airway lesion |
| Fixed airway obstruction | Flattening of both inspiratory and expiratory limbs | Fixed structural obstruction (goitre, post-intubation stenosis) |
Curve analysis is particularly valuable for identifying upper airway abnormalities and differentiating mechanical limitation from suboptimal patient effort — a distinction that numeric indices alone cannot reliably make.
Volume-Time Curves Validate Maneuver Completeness and Expiratory Duration
Volume-time curves provide temporal validation of forced expiratory maneuvers and are critical for confirming test adequacy. A valid maneuver requires rapid initiation, sustained exhalation, and achievement of an end-expiratory plateau — indicating that minimal additional volume change is occurring.
Acceptability Indicators
- Back-extrapolated volume within acceptable limits per ATS/ERS criteria
- Exhalation duration of ≥6 seconds in adults, or plateau achieved earlier
- No abrupt termination or premature cutoff of the expiratory effort
- Smooth, consistent curve without mid-maneuver artifacts
Failure to meet these criteria compromises the reliability of FVC and all derived indices, particularly in patients with severe obstruction who may require longer exhalation times.
Quality Control Grading Determines Whether Spirometry Data Is Clinically Actionable
Spirometry data is only interpretable when it meets strict acceptability and repeatability criteria defined by ATS/ERS standards. Modern systems apply automated quality grading based on multiple parameters, including start-of-test performance, absence of artifacts, and consistency across repeated maneuvers.
Repeatability Requirements
- Minimum of three acceptable maneuvers per test session
- FEV1 reproducibility within 150 mL between the two best efforts
- FVC reproducibility within 150 mL between the two best efforts
Common Technical Artifacts That Invalidate Maneuvers
- Cough during the first second — directly affects FEV1 measurement
- Hesitation or slow start — impacts peak flow and derived indices
- Variable effort — produces inconsistent curve shapes and values
- Air leaks around the mouthpiece — compromises volume accuracy
- Early termination — underestimates FVC and affects ratio calculations
Quality grading ensures that reported values reflect physiological reality rather than technical variability. Without verified quality grades, even accurate devices cannot produce reliable clinical data.
Bronchodilator Response Testing Quantifies Reversibility Using Absolute and Relative Thresholds
Bronchodilator response testing evaluates the degree of reversibility in airflow limitation by comparing pre- and post-bronchodilator spirometry values. Modern output includes both absolute changes (in litres) and percentage changes relative to baseline, allowing standardized assessment of reversibility.
Clinically Significant Response Criteria
- Increase in FEV1 or FVC of ≥12% from baseline
- Absolute increase of ≥200 mL
- Both criteria must be met simultaneously to define a significant response
These thresholds indicate reversible airway obstruction and support differentiation between conditions characterized by variable versus fixed airflow limitation. Interpretation must also consider baseline severity — smaller absolute changes may still carry clinical significance in patients with substantially reduced lung volumes.
Environmental Compensation and Calibration Protocols Directly Affect Measurement Accuracy
Spirometry accuracy depends on proper calibration and correction for environmental conditions, including temperature, pressure, and humidity. Modern devices apply BTPS (Body Temperature and Pressure, Saturated) correction to convert measured volumes to physiological conditions within the lungs, ensuring reported values are clinically meaningful regardless of ambient conditions at the time of testing.
Critical Calibration Considerations
- Daily calibration verification using a standardized 3-litre calibration syringe
- Sensor drift monitoring and periodic correction or recalibration
- Barometric pressure adjustment for altitude or weather changes
- Temperature stabilization of the device prior to testing sessions
Failure to maintain calibration introduces systematic error, particularly in volume measurements such as FVC — undermining interpretation even when patient effort and technique are optimal.
Diagnostic-Grade Spirometers Differ from Screening Devices in Signal Fidelity and Interpretive Depth
Not all spirometers are equivalent in clinical value. Diagnostic-grade systems provide higher resolution airflow measurement, comprehensive quality control, and full interpretive datasets compared to screening-level devices. The distinction matters when data is used to inform clinical decisions rather than simply flag patients for further assessment.
| Feature | Screening Devices | Diagnostic Systems |
|---|---|---|
| Sensor precision | Lower resolution | High-resolution flow sensing |
| Curve analysis | Limited or absent | Full flow-volume and volume-time curves |
| Quality control | Minimal | Automated grading and maneuver validation |
| Reference modeling | Basic % predicted only | LLN and z-score integration |
| Clinical application | Initial screening | Diagnosis and longitudinal monitoring |
Selection of device type directly impacts diagnostic confidence and data reproducibility over time. In settings where spirometry informs treatment decisions, diagnostic-grade capability is not optional.
Integration with Digital Systems Enables Longitudinal Pulmonary Function Analysis
Modern spirometry output is designed for structured integration with electronic medical record (EMR) systems, enabling longitudinal tracking of pulmonary function across multiple visits. Data standardization allows consistent comparison over time, which is essential for monitoring disease progression, evaluating treatment response, and detecting functional decline in at-risk populations.
- Trend analysis of FEV1 decline to assess disease progression rate against expected age-related loss
- Automated comparison against prior baselines with flagging of clinically significant changes
- Centralized storage of curve data for retrospective review and audit
Longitudinal consistency requires standardized testing protocols across visits. Variation in technique, time of day, or device calibration between sessions can introduce artifact that mimics clinical change.
Common Interpretation Errors Arise from Misuse of Statistical Thresholds
Incorrect interpretation of spirometry data often results from failure to apply statistical models correctly, or from disregarding maneuver quality when reporting values. These errors can lead to misdiagnosis, unnecessary treatment, or missed disease in clinical practice.
The Most Critical Errors in Clinical Practice
- Using fixed cutoffs (e.g., FEV1/FVC < 0.70) instead of LLN-based thresholds
- Ignoring z-scores in favour of percent predicted alone
- Interpreting results without verifying test quality grades
- Over-reliance on FEF25–75 as a primary diagnostic marker despite its high variability
- Failure to analyze flow-volume loop morphology alongside numeric values
- Accepting results from fewer than three acceptable maneuvers
Accurate interpretation requires integration of all available data elements: curves, statistical outputs, quality indicators, and clinical context. No single index should be interpreted in isolation.
Device Selection Criteria Must Prioritize Measurement Validity and Standards Compliance
Selection of a spirometry system must be based on technical performance, standards compliance, and integration capabilities. Choosing a device based on convenience or cost alone introduces variability that limits clinical utility and may compromise the reliability of longitudinal data.
Evaluation Criteria for Clinical Settings
- Compliance with current ATS/ERS technical standards for signal acquisition and reporting
- Availability of LLN and z-score–based interpretation with validated reference equations
- High-fidelity flow sensor technology with minimal drift over time
- Automated quality assurance features including maneuver grading and real-time feedback
- Compatibility with Canadian clinical workflows and EMR documentation systems
BOMImed provides spirometry and pulmonary diagnostic solutions within a broader portfolio of medical equipment in Canada, with a focus on clinically reliable measurement and system integration. BOMImed's spirometry offerings are designed to support accurate airflow and volume measurement consistent with recognized pulmonary testing standards, structured data output including key spirometric indices and graphical representations, and integration into clinical workflows where consistent documentation and repeatability are required.
As a Canadian-based provider of medical and veterinary diagnostic equipment, BOMImed emphasizes equipment reliability, service support, and alignment with clinical operational needs.
Frequently Asked Questions: Spirometry Data Interpretation
What is the role of z-scores in spirometry interpretation?
Z-scores quantify how far a measurement deviates from the predicted mean for a given age, sex, height, and ethnicity, allowing statistically valid classification of normal versus abnormal results without relying on arbitrary fixed thresholds.
Why is LLN preferred over percent predicted in spirometry?
The Lower Limit of Normal accounts for population variability across age groups and demographics, reducing misclassification errors. Fixed percent-predicted cutoffs overdiagnose obstruction in older adults and underdiagnose it in younger patients with early disease.
What defines an acceptable spirometry maneuver?
An acceptable maneuver includes rapid initiation at total lung capacity, absence of cough or other artifacts during the first second, sustained exhalation of at least 6 seconds or until a clear plateau is achieved, and reproducibility across a minimum of three attempts with FEV1 and FVC within 150 mL of each other.
How is airflow obstruction identified on spirometry?
Airflow obstruction is identified when the FEV1/FVC ratio falls below the Lower Limit of Normal — corresponding to a z-score of less than −1.64 — indicating that airflow limitation is statistically abnormal relative to the reference population.
What constitutes a significant bronchodilator response?
A clinically significant bronchodilator response requires both a ≥12% increase in FEV1 or FVC from baseline and an absolute increase of ≥200 mL. Both criteria must be met simultaneously to confirm reversibility.
Why is FEF25–75 considered less reliable as a standalone diagnostic marker?
FEF25–75 has high variability, is effort-dependent, and has wide confidence intervals in reference populations. These characteristics limit its diagnostic specificity as a standalone metric, though it may provide supplementary information when interpreted in context.
What is BTPS correction in spirometry?
BTPS (Body Temperature and Pressure, Saturated) correction adjusts measured airflow volumes to reflect the conditions inside the lungs, ensuring that reported values represent physiological reality rather than ambient environmental conditions at the time of testing.
How many maneuvers are required for reliable spirometry results?
At least three acceptable and reproducible maneuvers are required per ATS/ERS standards. FEV1 and FVC must each be reproducible within 150 mL across the best attempts to meet minimum repeatability requirements.
BOMImed Spirometry Solutions for Canadian Clinical Settings
BOMImed offers diagnostic-grade spirometry systems designed for accurate measurement, ATS/ERS–compliant output, and seamless integration into Canadian clinical workflows. Explore our spirometry portfolio or contact our team for clinical support.
View Spirometry Systems →