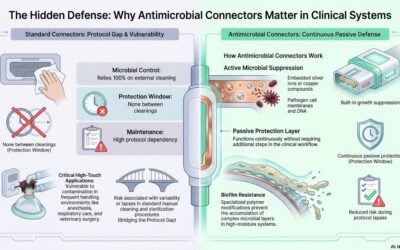
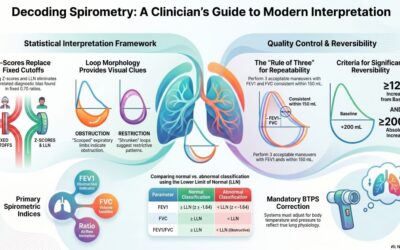
Professional spirometry systems and home spirometry tools serve the same core purpose but operate under distinct conditions, expectations, and performance thresholds. Clinical systems measure respiratory performance with tightly controlled calibration standards, guided workflows, and specialized components. Home spirometry introduces accessibility by enabling a spirometry test at home, but with inevitable trade-offs in precision, reliability, and data interpretation.
Clear distinctions between these categories shape how clinicians monitor disease, how patients track symptoms, and how organizations evaluate respiratory equipment. Understanding their differences is critical for selecting the correct method for diagnosis, monitoring, or ongoing management.
Spirometry System Functional Purpose and Intended Use
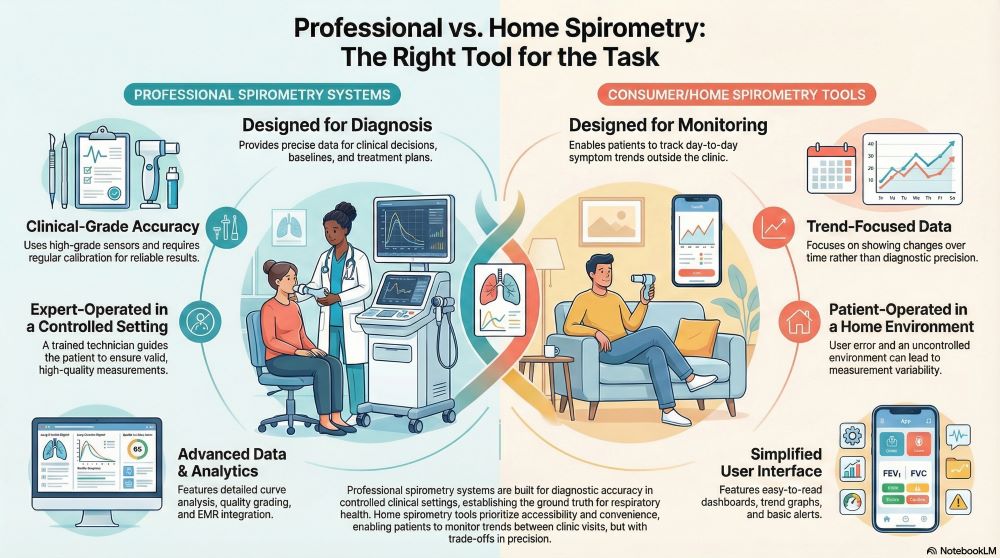
Professional systems are designed for diagnostic-level precision in controlled settings. Their role centers on establishing baselines, confirming respiratory disorders, and guiding treatment plans. These systems anchor pulmonary evaluation because their accuracy supports clinical decisions with narrow error tolerances.
Home spirometry expands access by enabling patients to track trends outside the clinic. Portable spirometry machines allow at-risk or chronically managed populations to monitor day-to-day changes without relying on appointment schedules. While this supports long-term visibility, it does not replace the standardization required for diagnostic use.
The difference in intended use reflects the environment in which measurements are taken. Clinical settings prioritize accuracy. At-home spirometry prioritizes convenience.
Spirometry Hardware Design and Measurement Precision
Professional spirometry systems use high-grade sensors, reinforced flow measurement chambers, and advanced signal processing hardware. These components limit external interference and provide consistency across repeated tests. Device housings and airflow paths are engineered for minimal turbulence and controlled resistance, supporting reliable calculations of FEV1, FVC, PEFR, and related indices.
Home spirometry devices rely on compact electronics and simplified flow channels to reduce cost and size. The goal is usability rather than absolute precision. Smaller sensors face wider variance because environmental conditions, airflow inconsistencies, and handling differences create more noise within the measurement process. Portable spirometry machines improve durability, but their miniaturized architecture remains less controlled than professional models.
The performance gap is not a limitation of consumer technology but a reflection of engineering priorities. Professional systems optimize for accuracy; consumer tools optimize for access.
Calibration and Quality Control Requirements
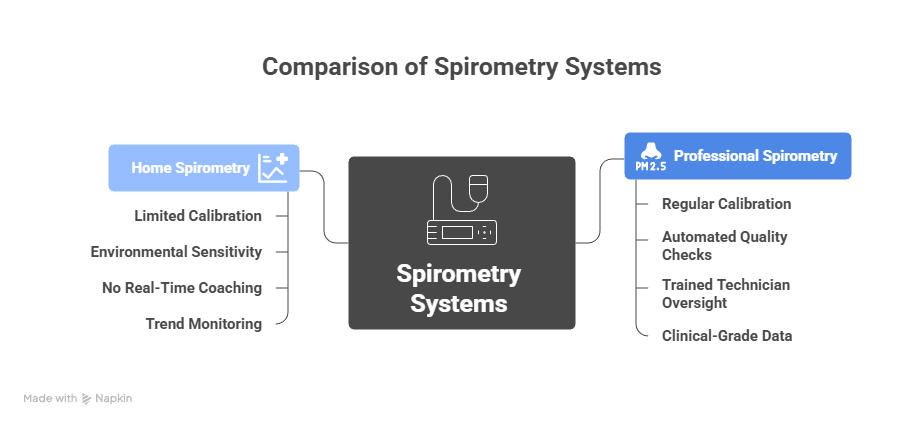
Professional spirometry equipment undergoes regular calibration using standardized syringes and facility protocols. Many clinical systems incorporate automated checks for leak detection, temperature compensation, and flow stability. These safeguards reduce the risk of drift over time and maintain predictable measurement conditions.
Home devices rarely include formal calibration frameworks. Some compensate through automated internal recalibration, but these mechanisms function within a limited range. Without controlled calibration procedures, the user’s environment introduces more variability. Improper technique further compounds the issue, as home users do not benefit from the in-person coaching provided by trained technicians.
The calibration difference shapes how clinicians interpret results. Professional results stand as baseline data. Home spirometry readings function best as trend indicators rather than precise diagnostic markers.
Testing Environment and Operator Skill
Clinical spirometry requires trained personnel who guide patients through each step of the maneuver. They ensure correct posture, mouthpiece positioning, inhalation depth, and exhalation force. The operator’s ability to recognize suboptimal efforts prevents the inclusion of flawed data.
At-home spirometry removes the trained operator. Users may perform a spirometry test at home with varying levels of technique, which affects the reproducibility of their results. Instructions built into portable spirometry machines assist with prompts, animations, or sound cues, but these aids cannot fully replace hands-on coaching. User error remains a leading factor in inaccurate home readings.
Professional environments control noise, temperature, airflow, and patient positioning. Home environments introduce uncontrolled variables that influence measurement stability. The gap in environmental control is a fundamental reason professional systems maintain higher accuracy standards.
Spirometry Software Capabilities and Data Interpretation
Professional spirometry software provides detailed curve analysis, predicted value sets, quality grading, effort validation, and longitudinal reporting. Many systems integrate with electronic medical records, allowing clinicians to track changes precisely over time. Advanced visualization tools illuminate subtle declines that might otherwise go unnoticed.
Home spirometry tools feature simplified dashboards designed for patient comprehension. Their focus is on clarity rather than the full analytic range required for diagnostic interpretation. Trend graphs, threshold alerts, and symptom reminders guide patient self-monitoring. While these features support engagement, they lack the depth of clinical analysis.
The difference in software sophistication aligns with regulatory expectations. Clinical systems require robust interpretations compatible with medical oversight. Home systems require accessible insights compatible with daily self-care.
Regulatory Classification and Performance Standards
Professional spirometry systems fall under stringent medical device classifications that require validated performance reporting, repeatability standards, and controlled manufacturing processes. Compliance ensures that measurements meet defined accuracy thresholds under diverse testing conditions.
Home spirometry devices occupy a different regulatory track focused on wellness, remote monitoring, or supplemental patient support. Their classifications allow broader accessibility but do not impose the same precision requirements as diagnostic systems.
This divergence shapes the real-world expectations of each product category. Professional systems are held to clinical-grade standards. Home devices are held to consumer-accessibility standards.
Impact on Clinical Decision-Making
Diagnostic accuracy relies on professional spirometry results. Treatment adjustments, specialist referrals, medication changes, and baseline assessments all require the stability provided by calibrated clinical equipment. These foundational tests cannot be replaced by consumer alternatives.
Home spirometry supports clinical decision-making indirectly by supplying interim data. For chronic respiratory conditions, daily or weekly readings contextualize symptoms and help clinicians detect trends before they escalate. When patients perform regular at-home spirometry, clinicians gain visibility into fluctuations that would not appear during isolated visits.
The two systems function in parallel rather than in competition. Professional spirometry provides the ground truth. Home spirometry supplies additional context.
Data Continuity and Remote Monitoring
Healthcare providers increasingly rely on remote monitoring platforms that aggregate data from portable spirometry machines. These systems allow clinicians to observe patterns across extended periods. Continuous data collection improves the clinician’s ability to identify deviations from normal patterns, particularly in conditions with variable symptom profiles.
Professional spirometry remains the reference point for interpreting these trends. Differences in device calibration, environment, and user technique require a consistent clinical baseline for comparison. Without this anchor, remote readings lose interpretive value.
The integration of home spirometry with clinical workflows marks a shift toward hybrid monitoring models. Each category reinforces the other, but professional systems retain interpretive authority.
Cost Differentiation – Professional vs At-Home Spirometry Ez
Professional spirometry systems reflect their precision-driven engineering, advanced software, and regulated manufacturing processes. Their costs include calibrators, accessories, maintenance requirements, and facility-grade components. These expenses are justifiable because clinical accuracy produces long-term diagnostic and treatment value.
Home spirometry devices offer lower entry costs, appealing to patients who require consistent monitoring rather than diagnostic-level precision. Portable spirometry machines strike a balance between affordability and capability by minimizing hardware complexity while preserving core functionality.
The cost difference influences adoption patterns. Clinics invest in accuracy. Patients invest in convenience.
Portability and User Convenience
Portability defines the consumer spirometry category. Lightweight construction, rechargeable power, and simplified interfaces make it practical for users to complete a spirometry test at home or while traveling. This mobility encourages adherence to routine monitoring schedules and supports disease management outside clinical environments.
Professional systems prioritize stability over mobility. Larger housings, tethered sensors, and integrated calibration components maintain measurement control. While some professional-grade portable spirometry machines exist, they remain heavier and more complex than consumer models because they maintain stricter measurement tolerances.
This trade-off reinforces the distinction between clinical precision and patient accessibility.
Measurement Variability and Interpretation Risk
Home spirometry devices introduce broader measurement variability due to technique inconsistency, environmental factors, and sensor limitations. Minor deviations in inhalation depth or exhalation force significantly alter FEV1 and FVC results, creating fluctuations unrelated to physiological changes.
Professional spirometry systems reduce this variability through operator coaching and environmental control. Their ability to detect suboptimal effort prevents inaccurate readings from entering medical records. This quality assurance is essential for clinical decision-making and long-term trend tracking.
Clinicians using home-generated data account for these limitations by focusing on directional trends rather than isolated values. The risk profile of home spirometry reinforces the importance of anchoring interpretation to professional baselines.
Longevity, Maintenance, and Lifecycle Reliability
Professional spirometry systems are built for continuous use within clinical environments. Their components withstand repeated sterilization, daily testing cycles, and long-term operational stress. Facilities schedule preventative maintenance to preserve sensor accuracy and extend equipment longevity. This structured lifecycle ensures consistent performance throughout high-volume clinical usage.
Home spirometry devices operate in lower-demand environments. Their sensors, battery systems, and housings are engineered for periodic use, not continuous clinical throughput. While durable, they generally offer shorter lifespans and rely on user-dependent care. Replacement intervals tend to arrive sooner due to lighter construction and fewer maintenance mechanisms. The longevity gap reflects the operational expectations of each device category.
Reliability over time follows these construction differences. Clinical systems maintain stable accuracy for years under managed conditions. Home systems may experience drift as components wear, reinforcing the importance of professional baselines for long-term assessments.
Data Connectivity and Clinical Integration
Professional spirometry systems integrate with electronic health record ecosystems, respiratory information systems, and hospital networks. Their connectivity supports structured data storage, compliance auditing, and continuous care coordination. Standardized data formats ensure that results maintain clinical-grade traceability across departments and patient encounters.
Home spirometry devices typically rely on Bluetooth connections to smartphones or tablets, uploading information through patient-facing apps or cloud portals. These systems focus on personal tracking rather than enterprise-level integration. Some advanced models interface with remote monitoring platforms used by clinics, but the connection usually requires intermediary software rather than direct EHR integration.
This dichotomy shapes how clinicians interact with spirometry data. Professional integrations create complete respiratory profiles tied to patient records. Home integrations create supplemental data streams that clinicians interpret alongside core clinical results.
User Experience Design and Accessibility
Professional spirometry interfaces are designed for trained technicians who understand maneuver sequences and quality grading. These systems emphasize precision feedback, curve displays, and advanced functions that support expert use. Their complexity is intentional because it supports diagnostic-level oversight.
Home spirometry tools prioritize simplicity. The interface directs users through steps with minimal decision-making. Graphs emphasize trends rather than detailed waveform interpretation. This design philosophy removes barriers to daily monitoring and supports broader accessibility among patients with varying comfort levels.
Accessibility plays a functional role in supporting adherence. Patients who can reliably perform at-home spirometry contribute more meaningful trend data. User experience design therefore has measurable influence on monitoring success, even when accuracy remains below clinical standards.
Clinical Applications and Use-Case Scenarios
Professional spirometry systems anchor diagnosis and comprehensive pulmonary evaluation. They are used during routine lung function testing, preoperative assessments, occupational surveillance, and the monitoring of chronic respiratory disorders. Their reliability supports determination of disease severity, progression rates, and therapeutic impact.
Home spirometry expands ongoing management. Users perform a spirometry test at home to identify early deviations, monitor day-to-day stability, and provide clinicians with broader visibility between visits. These tools are valuable for conditions characterized by fluctuations or exacerbations, where early detection can influence outcomes.
While home spirometry supports ongoing oversight, it cannot fulfill roles that require validated diagnostic precision. Its utility lies in supplementing clinical evaluation, not replacing it.
Risk Management and Data Interpretation Safeguards
Professional spirometry incorporates built-in safeguards to ensure that only valid, high-quality maneuvers are accepted. Automated grading systems reject inconsistent efforts, encourage repeat attempts, and highlight anomalies. This reduces the likelihood of misinterpretation and helps clinicians maintain confidence in the final data set.
Home spirometry lacks comprehensive safeguards. Even when devices include quality prompts, users may unknowingly submit suboptimal measurements. Without technician oversight, results may reflect technique variability rather than physiological changes. For clinicians, this reinforces the need to interpret home readings within a broader context rather than treating them as definitive values.
These limitations do not diminish the usefulness of home spirometry. Instead, they define the parameters within which it can function safely and effectively.
Influence of Device Complexity on Learning Curve
Professional spirometry presents no learning curve for patients because operators manage the procedure. Technicians guide each step, correct mistakes, and ensure consistent execution. This structure eliminates user-driven variability during the testing process.
Home spirometry shifts the learning curve onto the patient. Users must master inhalation depth, sealing technique, posture, and exhalation effort. Improper practice reduces consistency and can obscure meaningful trends. Educational resources embedded in portable spirometry machines help mitigate this challenge but cannot fully replicate technician expertise.
The learning curve highlights one of the clearest distinctions between the two categories: professional systems isolate users from procedural complexity; home systems require users to manage it.
Role of At-Home Spirometry in Telehealth Models
As telehealth expands, at-home spirometry plays a growing role in remote disease management. Daily or weekly measurements support proactive care models by offering continuous visibility into respiratory patterns. These readings allow clinicians to intervene earlier, adjust therapies sooner, and maintain engagement outside traditional appointments.
Professional spirometry remains central to telehealth verification. When home readings signal a significant change, clinical retesting provides definitive confirmation. This dual-system approach strengthens telehealth workflows by combining broad monitoring with precise diagnostics.
Telehealth underscores the complementary nature of home and professional tools rather than a competitive dynamic between them.
Specialized Features That Differentiate Professional Spriometry Equipment
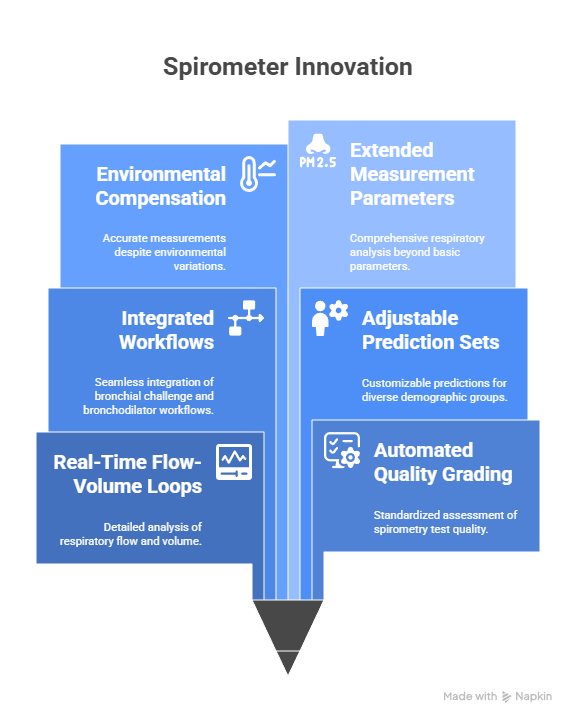
Professional spirometry systems include advanced features designed for comprehensive pulmonary analysis. These often include:
- Real-time flow-volume loops with detailed curve morphology
- Automated quality grading based on standardized criteria
- Integrated bronchial challenge and pre/post bronchodilator workflows
- Adjustable prediction sets for demographic variability
- Environmental compensation for temperature, pressure, and humidity
- Extended measurement parameters beyond FEV1 and FVC
These features allow clinicians to identify subtle abnormalities and track disease trajectories with high confidence. The sophistication of these systems enables deeper interpretation of respiratory mechanics.
Home spirometry tools focus on core indicators. Their feature sets typically include:
- Basic FEV1 and FVC measurements
- Trend graphs over days or weeks
- Basic quality prompts
- Alert thresholds for declines from baseline
- Simple user dashboards
The contrast reveals two distinct design philosophies: comprehensive diagnostics versus accessible self-monitoring.
Durability Standards and Infection Control
Professional spirometry systems operate under strict infection control standards. Clinics rely on disposable mouthpieces, antimicrobial components, sterilization protocols, and robust housings designed to withstand frequent cleaning. These standards ensure safety within repeated patient-use environments.
Home spirometry eliminates shared usage, reducing infection concerns but still requiring proper hygiene. Portable spirometry machines typically use washable parts or replaceable mouthpieces designed for individual users. They are not built for the intense cleaning cycles required in clinical settings, but they do maintain safety for home use when handled correctly.
Durability standards directly reflect the operational environments in which these devices function.
Interpreting Variability in Home Spirometry Data
Variability is inherent in home-generated spirometry due to differences in technique, timing, and environment. Clinicians interpret these readings by focusing on directional consistency rather than precise values. A single low reading may reflect poor technique, but a pattern of declining results may reflect genuine physiological change.
Professional spirometry remains the interpretive reference point. When home spirometry signals potential declines, clinical testing confirms or refutes the trend. This process ensures that management decisions remain grounded in validated data.
Understanding variability helps set proper expectations for at-home spirometry users. The goal is trend recognition, not diagnostic precision.
Value of Home Spirometry in Chronic Disease Management
At-home spirometry provides substantial value for chronic conditions marked by dynamic symptom patterns. Routine readings help patients understand their baseline and observe deviations early. This awareness supports adherence to care plans and improves communication with clinicians.
Portable spirometry machines enable this routine tracking with minimal burden. Their convenience helps patients maintain consistent monitoring schedules, which improves the usefulness of collected data. While the readings do not replace clinical-grade testing, they enhance the continuity of care.
This role in chronic disease management contributes to the growing adoption of home spirometry across diverse care models.
Integrating Professional and Home Spirometry in Long-Term Care
Long-term respiratory care benefits from a hybrid approach that leverages the strengths of both systems. Professional spirometry establishes baselines, diagnoses conditions, and anchors the clinical record. Home spirometry fills the gaps between visits, providing supplemental insights that reflect real-world fluctuations.
This hybrid framework enables more refined monitoring, earlier intervention, and improved patient engagement. Clinical outcomes depend on both accuracy and continuity; professional and home spirometry contribute differently to these goals.
The integration of both tools reflects a shift toward distributed care models where precision and accessibility work in tandem.
FAQ’s
How accurate is a spirometry test at home?
A spirometry test at home offers reliable trend monitoring but lacks the precision of professional systems. Technique, environment, and device limitations contribute to variability.
Can home spirometry replace clinical spirometry tests?
Home spirometry cannot replace clinical testing. Professional systems remain the standard for diagnosis, baseline establishment, and treatment decision-making.
What is the benefit of using a portable spirometry machine?
A portable spirometry machine supports daily or weekly monitoring, helping patients identify early changes and providing clinicians with broader context between visits.
Why are professional spirometry systems more accurate?
Professional systems use advanced sensors, controlled environments, calibration protocols, and technician oversight, all of which reduce measurement variability.
Is home spirometry useful for chronic respiratory conditions?
Yes. Home spirometry helps track fluctuations, supports symptom awareness, and enhances remote monitoring programs.
How should clinicians interpret home spirometry data?
Clinicians interpret home readings as directional indicators rather than definitive measurements, comparing them to professional baselines.
What features matter most in professional spirometry equipment?
Curve analysis, quality grading, validated calibration, advanced prediction sets, and environmental compensation are key differentiators.
Are portable spirometry machines durable enough for frequent use?
Portable devices suit regular home use but lack the industrial durability and long-term stability of professional systems.