Veterinary laser therapy is a noninvasive modality that uses targeted light energy to influence cellular activity, primarily for pain management, inflammation reduction, and tissue repair support. In practice, it functions as an adjunctive treatment integrated into broader medical or rehabilitation plans rather than a standalone solution.
Clinics do not deploy laser therapy as a general-purpose treatment. Its value depends on correct case selection, consistent dosing protocols, and alignment with existing services such as surgery, rehabilitation, and chronic care management. When implemented correctly, it becomes a repeatable, protocol-driven service that supports both patient outcomes and operational efficiency.
The clinical question is not whether laser therapy works in isolation, but whether the clinic can operationalize it in a controlled, repeatable way across its patient base.
Why the term “cold laser” creates confusion in equipment selection
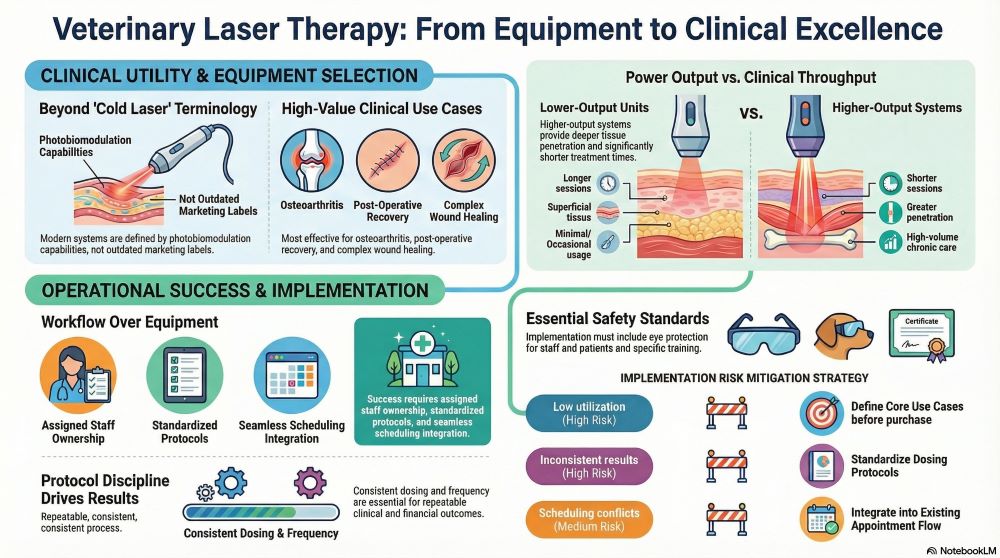
“Cold laser” is an outdated shorthand that refers to therapeutic lasers designed to avoid tissue ablation or cutting. While still widely used in marketing and conversation, the term does not accurately describe the range of modern veterinary systems available today.
Devices vary significantly in output power, wavelength combinations, delivery mechanisms, and software control. A low-output handheld unit used occasionally for wound care is fundamentally different from a higher-power system integrated into a rehabilitation or orthopedic workflow.
Treating all systems as interchangeable under the “cold laser” label leads to mismatched expectations. Clinics often underestimate the importance of treatment depth, dosing precision, and throughput capacity, all of which directly affect clinical and financial outcomes.
A more accurate framing is photobiomodulation equipment, where device capabilities must be evaluated based on intended use rather than terminology.
How photobiomodulation influences tissue response
Photobiomodulation works by delivering light at specific wavelengths that interact with cellular components, influencing metabolic activity and signaling pathways. The intended effect is to support tissue repair processes and modulate inflammation and pain perception.
The practical impact of this mechanism depends on several controllable variables:
- Wavelength determines tissue penetration depth
- Power output influences treatment time and energy delivery
- Application technique affects coverage and consistency
- Protocol selection determines dosing accuracy
- Tissue type alters absorption and response behavior
Clinics that treat laser therapy as a standardized, protocol-driven modality achieve more consistent outcomes than those using it sporadically or without structured dosing.
The mechanism is only as effective as the clinic’s ability to apply it correctly.
Which clinical use cases generate the most value
Laser therapy provides the most value when applied to conditions that require repeated treatment and align with existing service lines. It is most effective in scenarios where incremental improvement over time is expected and measurable.
High-value clinical applications typically include:
- Osteoarthritis and chronic joint pain management
- Postoperative recovery, particularly orthopedic procedures
- Soft tissue injuries such as strains and ligament involvement
- Wound healing support for complex or slow-healing cases
- Rehabilitation programs, including mobility and conditioning
- Neurologic recovery support in select cases
Not all use cases carry equal operational weight. Chronic conditions and rehabilitation programs tend to drive recurring visits, making them more predictable from both a clinical and revenue standpoint.
Short-term applications, such as post-surgical support, still provide value but are less impactful in building long-term utilization.
How laser therapy integrates into a veterinary workflow
Laser therapy succeeds when it is embedded into existing workflows rather than treated as an add-on service. Clinics that struggle with adoption often fail to assign ownership, standardize protocols, or allocate time effectively.
A functional workflow typically includes:
- Defined treatment protocols for common conditions
- Designated staff trained to administer treatments
- Scheduling integration with existing appointments
- Documentation of treatment parameters and outcomes
- Clear communication with pet owners about expectations
Integration is less about equipment capability and more about operational discipline. Even high-end systems underperform if they are not consistently used or properly scheduled.
Clinics that build structured protocols around repeatable conditions see significantly higher utilization rates.
Evaluating different types of veterinary laser equipment
Veterinary laser systems vary across several dimensions that directly affect usability and outcomes. Equipment selection should be based on clinical needs, staff capacity, and anticipated case volume.
Core differences between device categories
| Feature | Lower-Output Units | Higher-Output Systems |
|---|---|---|
| Power Output | Lower energy delivery | Higher energy delivery |
| Treatment Time | Longer sessions | Shorter sessions |
| Depth Capability | More superficial | Greater penetration |
| Cost | Lower initial investment | Higher upfront cost |
| Throughput | Limited volume capacity | Designed for higher usage |
Lower-output systems may be sufficient for clinics with minimal usage or limited case diversity. Higher-output systems are more appropriate for practices with orthopedic, rehabilitation, or high-volume chronic care cases.
Additional evaluation criteria
Clinics should assess:
- Ease of use and training requirements
- Software-driven protocols versus manual control
- Applicator design and ergonomics
- Durability and service support
- Ability to scale with practice growth
Equipment selection is ultimately a capacity decision. The right system is one that aligns with both current demand and realistic future usage.
What clinics often misunderstand about treatment protocols
Laser therapy outcomes are highly dependent on dosing consistency, yet many clinics rely on inconsistent or generalized protocols. This creates variability in results and undermines confidence in the modality.
Common misunderstandings include:
- Assuming one protocol fits all cases
- Underestimating the importance of treatment frequency
- Applying insufficient energy to reach target tissue
- Failing to track outcomes and adjust protocols
- Using the device intermittently rather than systematically
Clinics that standardize protocols for common conditions—such as osteoarthritis or postoperative recovery—see more reliable outcomes and stronger client satisfaction.
Protocol discipline is the difference between occasional success and repeatable performance.
Safety considerations that cannot be overlooked
Laser therapy is generally considered low-risk, but improper use can still create safety issues for both patients and staff. Clinics must establish clear safety practices as part of implementation.
Key safety considerations include:
- Eye protection for staff and patients
- Avoidance of direct exposure to sensitive areas
- Proper training on device operation
- Adherence to manufacturer guidelines
- Controlled treatment environments
Risk is not eliminated by the “cold” designation. Even non-ablative systems require controlled usage to prevent unintended exposure or misuse.
A structured safety protocol is a baseline requirement, not an optional precaution.
How clinics evaluate whether laser therapy fits their practice
Laser therapy is not universally appropriate for every clinic. The decision should be based on alignment with existing services, patient demographics, and operational capacity.
Key decision criteria
- Volume of chronic pain or orthopedic cases
- Presence of rehabilitation or recovery-focused services
- Staff availability and training capacity
- Willingness to standardize protocols
- Ability to support repeat-visit treatment models
Clinics with a high proportion of acute, one-time visits may see limited value. Those with ongoing care relationships tend to benefit more significantly.
A clear understanding of the practice model is required before making an investment.
Where equipment providers differentiate in the market
Not all veterinary laser systems deliver the same level of clinical usability or operational support. The most meaningful differentiation often comes from how well the system integrates into real-world workflows.
Key differentiators
- Pre-programmed treatment protocols
- Training and onboarding support
- Reliability and maintenance requirements
- User interface simplicity
- Scalability across multiple treatment types
For clinics evaluating solutions, providers that prioritize ease of use and structured implementation tend to produce better long-term adoption.
Positioning of BOMImed within the equipment landscape
BOMImed stands out by aligning equipment design with clinical workflow needs rather than focusing solely on technical specifications. Their approach emphasizes usability, training support, and integration into existing veterinary services.
This positioning matters because most adoption challenges are operational, not technical. Clinics benefit more from systems that are consistently used than from those with advanced features that remain underutilized.
What implementation challenges clinics should anticipate
Laser therapy adoption often fails due to operational gaps rather than equipment limitations. Clinics should anticipate and plan for these challenges before investing.
Common implementation risks
- Lack of staff ownership or accountability
- Inconsistent protocol application
- Poor scheduling integration
- Underestimating training requirements
- Limited client education and buy-in
Risk matrix for implementation
| Risk | Impact | Likelihood | Mitigation |
|---|---|---|---|
| Low utilization | High | Moderate | Define core use cases before purchase |
| Inconsistent results | High | High | Standardize protocols |
| Staff resistance | Medium | Moderate | Provide structured training |
| Scheduling conflicts | Medium | High | Integrate into appointment flow |
| Client hesitation | Medium | Moderate | Communicate treatment expectations |
Successful implementation requires planning beyond the initial purchase decision.
How client perception influences adoption and retention
Client perception plays a significant role in whether laser therapy becomes a recurring service within a clinic. Pet owners must understand both the purpose and expected outcomes of treatment.
Clear communication should focus on:
- Realistic expectations for improvement
- Need for multiple sessions
- Role within a broader treatment plan
- Observable benefits over time
Clinics that present laser therapy as a structured, evidence-informed service rather than a novelty achieve stronger client acceptance and compliance.
Trust is built through consistency and clarity, not marketing language.
FAQ’s
What is the difference between cold laser and laser therapy in veterinary medicine?
Cold laser is a legacy term referring to non-ablative therapeutic lasers, while modern veterinary laser therapy encompasses a broader range of photobiomodulation devices with varying power and capabilities.
How long does a typical veterinary laser therapy session take?
Session length varies based on device power and treatment area, but higher-output systems generally reduce treatment time while delivering equivalent or greater energy.
Is laser therapy safe for animals?
Laser therapy is considered safe when used correctly, with proper training, controlled protocols, and appropriate protective measures.
How many treatments are usually required?
Most conditions require multiple sessions, particularly chronic issues such as osteoarthritis, where ongoing treatment may be part of long-term management.
Can laser therapy replace medications or surgery?
Laser therapy is typically used as a complementary modality and does not replace core treatments such as surgery or pharmacologic management.
Do all veterinary clinics benefit from adding laser therapy?
Clinics with higher volumes of chronic pain, orthopedic, or rehabilitation cases tend to benefit most from implementation.
What should clinics look for when choosing a laser device?
Clinics should evaluate power output, usability, protocol support, training resources, and alignment with their specific case mix.
Where veterinary laser therapy is heading
Veterinary laser therapy is moving toward more protocol-driven, integrated care models where consistency and workflow alignment define success more than device specifications. Clinics that treat it as a structured clinical service rather than an optional add-on will be positioned to extract the greatest long-term value.