In This Article
- Centralized Purchasing Models
- Independent Hospital Flexibility
- Total Cost of Ownership
- Utilization Rate
- Financing Structures
- Vendor Relationships
- Standardization vs. Customization
- Risk Distribution
- Data Availability
- Service Line Strategy
- Operational Integration
- The Role of BOMImed
- Capability Misalignment
- Lifecycle Planning
- Evaluation Framework
- Common Misconceptions
- FAQ
- Conclusion
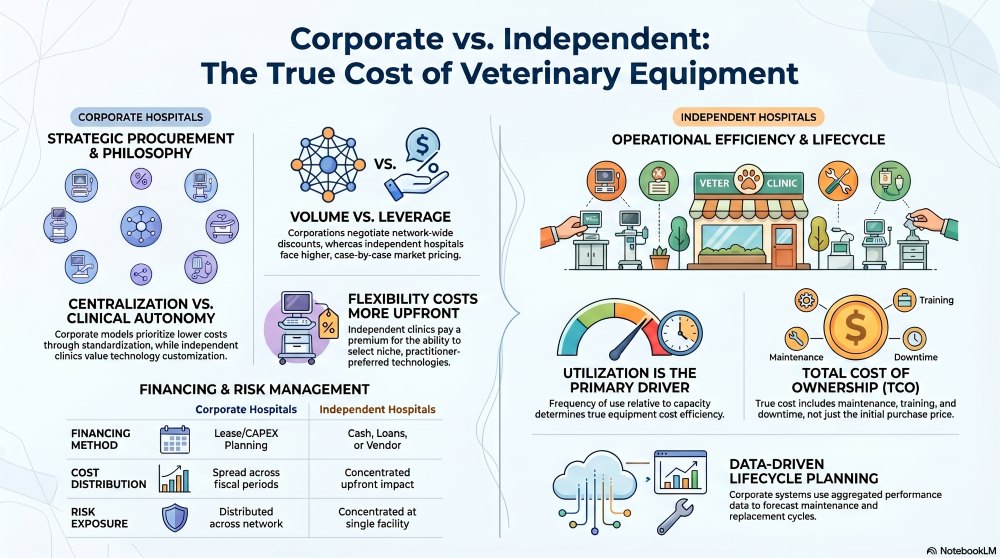
Veterinary networks compare equipment costs by aligning procurement strategy, capital allocation, and utilization expectations across hospital types. Corporate hospitals operate within centralized purchasing systems, while independent hospitals rely on localized decision-making with greater variability in pricing and timing. The result is not simply a pricing difference — it reflects structural differences in how equipment is selected, financed, deployed, and measured over time.
Centralized Purchasing Models Reduce Unit Cost but Increase Standardization Constraints
Corporate veterinary groups achieve lower per-unit equipment costs through centralized procurement. Volume-based contracts allow networks to negotiate discounted pricing, bundled service agreements, and extended warranties across multiple facilities. This model introduces consistency but reduces optionality — equipment selection is often limited to approved vendors and standardized configurations, even when clinical teams prefer alternatives.
Corporate procurement characteristics include:
- Multi-year vendor agreements tied to network-wide volume commitments
- Pre-approved equipment lists aligned with operational standards
- Bundled pricing for service, maintenance, and software updates
- Reduced negotiation at the individual hospital level
- Coordinated deployment schedules across regions
Lower acquisition cost is offset by reduced adaptability at the individual hospital level. Clinical autonomy becomes secondary to operational efficiency.
Independent Hospitals Pay Higher Upfront Costs but Retain Strategic Flexibility
Independent veterinary hospitals typically face higher equipment costs due to lower purchasing volume and limited negotiation leverage. Pricing variability is significant, depending on vendor relationships, timing, and geographic factors. This higher cost structure enables more precise alignment between equipment selection and clinical need. Decision-makers can evaluate technologies based on patient population, specialty focus, and practitioner expertise.
Independent procurement characteristics include:
- Vendor selection based on clinical preference rather than contracts
- Flexible timing for capital investment decisions
- Greater willingness to adopt niche or emerging technologies
- Negotiation occurring on a case-by-case basis
- Custom configurations tailored to specific workflows
This flexibility allows independent hospitals to differentiate services but introduces financial exposure if utilization does not justify the investment.
Total Cost of Ownership Determines True Cost Beyond Initial Purchase Price
Veterinary networks evaluate equipment costs using total cost of ownership (TCO), not just acquisition price. TCO incorporates lifecycle expenses, utilization rates, maintenance requirements, and operational impact. Corporate systems calculate TCO at scale using aggregated data across dozens or hundreds of hospitals. Independent hospitals must estimate TCO with less historical data, increasing uncertainty.
Core TCO components include:
- Initial purchase or lease cost
- Installation and training expenses
- Maintenance contracts and service frequency
- Software licensing and updates
- Consumables and replacement parts
- Equipment downtime and operational disruption
A lower purchase price does not guarantee lower TCO. High-maintenance equipment or underutilized systems can significantly increase long-term cost per procedure.
Utilization Rate Is the Primary Driver of Equipment Cost Efficiency
Equipment cost efficiency is determined by how frequently the equipment is used relative to its capacity. Corporate veterinary networks optimize utilization by distributing services across multiple hospitals or directing cases to higher-volume locations. Independent hospitals rely on internal case volume to justify equipment investment. Underutilization creates cost inefficiency regardless of acquisition price.
Utilization differences typically appear in:
- Imaging systems such as ultrasound or digital radiography
- Surgical equipment with specialized applications
- Monitoring and anesthesia platforms with varying patient volumes
Corporate systems may centralize high-cost equipment in regional hubs, while independent hospitals must decide whether to invest locally or refer cases externally.
Financing Structures Create Divergent Cost Profiles
Corporate veterinary networks often use structured financing models, including leasing, capital expenditure planning, and vendor-backed financing agreements. These models distribute cost over time and align expenses with revenue generation. Independent hospitals may use a mix of cash purchases, loans, or short-term financing, leading to more immediate financial impact.
| Factor | Corporate Hospitals | Independent Hospitals |
|---|---|---|
| Financing Method | Lease agreements, structured CAPEX planning | Cash purchase, loans, vendor financing |
| Cost Distribution | Spread across multiple fiscal periods | Concentrated upfront or short-term |
| Risk Exposure | Distributed across network | Concentrated at single facility |
| Approval Process | Centralized, multi-layer approval | Owner or small group decision-making |
| Flexibility | Low after contract commitment | High before purchase, limited after |
Financing decisions influence not only cost but also timing, risk tolerance, and equipment lifecycle management.
Vendor Relationships Shape Long-Term Cost Outcomes
Vendor strategy directly impacts both acquisition cost and long-term operational expense. Corporate networks often establish strategic partnerships with a limited number of manufacturers or distributors, securing favorable pricing and support terms. Independent hospitals maintain broader vendor diversity but may lack leverage for negotiating long-term service agreements.
Key vendor-related cost factors include:
- Service response time and availability
- Warranty coverage and extension options
- Software support and upgrade policies
- Training and onboarding resources
- Replacement part accessibility
A lower initial price from a less established vendor can result in higher long-term costs if service reliability is inconsistent.
Standardization Versus Customization Defines Equipment Strategy
Corporate veterinary groups prioritize standardization to ensure operational consistency across locations. Equipment models, interfaces, and workflows are aligned to simplify training and maintenance. Independent hospitals prioritize customization, selecting equipment that aligns with specific clinical approaches or specialties.
This distinction creates measurable differences:
- Standardization reduces training complexity and service variability
- Customization enables differentiation and specialized care delivery
- Standardized systems are easier to scale across multiple locations
- Customized systems require more individualized support and expertise
Neither approach is inherently superior. The effectiveness depends on operational goals and patient care strategy.
Risk Distribution Alters Equipment Investment Decisions
Corporate networks distribute financial risk across multiple hospitals, allowing for more aggressive investment in high-cost equipment. A single underperforming asset has limited impact on overall network performance. Independent hospitals carry full financial responsibility for each equipment decision. This constraint often leads to more conservative purchasing behavior.
Risk considerations include:
- Volume uncertainty for new services
- Technology obsolescence over time
- Maintenance unpredictability
- Staff training requirements
- Market demand fluctuations
Corporate systems absorb these risks through scale. Independent hospitals must mitigate risk through careful evaluation and phased investment.
Data Availability Improves Cost Modelling Accuracy in Corporate Systems
Corporate veterinary networks rely on aggregated performance data to evaluate equipment cost efficiency. Metrics such as cost per procedure, utilization rate, and maintenance frequency are tracked across multiple locations. Independent hospitals typically operate with limited datasets, relying on projections rather than historical benchmarks.
Data-driven evaluation enables corporate systems to:
- Identify underperforming equipment across locations
- Optimize allocation of high-cost assets
- Forecast maintenance and replacement cycles
- Adjust procurement strategy based on real-world outcomes
Limited data increases uncertainty in independent settings, requiring more conservative financial assumptions.
Service Line Strategy Influences Equipment Investment Priorities
Corporate veterinary networks align equipment purchases with broader service line strategies, such as expanding specialty care or increasing diagnostic capabilities across regions. Independent hospitals align equipment investment with local demand and practitioner expertise.
Service line alignment affects:
- Selection of advanced diagnostic equipment
- Investment in surgical capabilities
- Adoption of emerging technologies
- Integration of equipment into patient workflows
Corporate systems prioritize scalability, while independent hospitals prioritize immediate clinical impact.
Operational Integration Determines Realized Equipment Value
Equipment value is realized through integration into daily clinical workflows. Corporate systems often deploy standardized training programs and operational protocols to ensure consistent usage. Independent hospitals rely on internal adoption, which can vary based on staff experience and familiarity.
Operational integration factors include:
- Staff training and competency development
- Workflow alignment with existing processes
- Integration with practice management systems
- Ongoing usage monitoring and optimization
Poor integration reduces utilization and increases cost per use, regardless of acquisition strategy.
The Role of BOMImed in Equipment Cost Evaluation
Specialized distributors such as BOMImed influence cost comparison by providing tailored equipment solutions, clinical guidance, and support structures that differ from large-scale procurement models. These providers often bridge the gap between corporate standardization and independent customization. BOMImed operates within a model that emphasizes clinical alignment and product specialization. Equipment selection is guided by application-specific requirements rather than broad standardization mandates.
Key contributions in cost evaluation include:
- Matching equipment specifications to clinical use cases
- Providing detailed product knowledge for informed decision-making
- Offering support structures that reduce operational friction
- Enabling access to specialized technologies not always included in corporate contracts
This approach can improve cost efficiency by reducing misalignment between equipment capability and actual usage.
Misalignment Between Equipment Capability and Clinical Need Drives Cost Inefficiency
The most common cost inefficiency occurs when equipment capabilities exceed actual clinical requirements. Corporate systems mitigate this risk through standardization, while independent hospitals must evaluate alignment on a case-by-case basis.
Over-specification leads to:
- Higher upfront costs without proportional revenue increase
- Underutilized advanced features
- Increased maintenance complexity
- Longer training requirements
Under-specification creates different risks, including limited diagnostic capability and reduced service offerings. Effective cost comparison requires precise alignment between equipment functionality and expected clinical use.
Lifecycle Planning Determines Long-Term Financial Impact
Equipment cost must be evaluated across its entire lifecycle, including acquisition, operation, maintenance, and replacement. Corporate networks plan lifecycle stages across multiple hospitals, allowing for coordinated upgrades and phased replacements. Independent hospitals often manage lifecycle planning reactively, replacing equipment based on failure or obsolescence.
Lifecycle considerations include:
- Expected useful life of the equipment
- Maintenance cost escalation over time
- Technology advancement and obsolescence risk
- Residual value or trade-in potential
- Timing of replacement relative to revenue generation
Proactive lifecycle planning reduces unexpected costs and improves financial predictability.
Comparative Evaluation Framework for Decision-Makers
Veterinary networks use structured frameworks to compare equipment costs across hospital types. These frameworks integrate financial, operational, and clinical considerations.
| Evaluation Factor | Key Question | Impact on Cost Decision |
|---|---|---|
| Utilization | Will the equipment be used consistently? | Determines cost per use |
| Clinical Fit | Does it match patient and service needs? | Prevents over- or under-specification |
| Financing Structure | How is the purchase funded? | Affects cash flow and risk |
| Vendor Support | Is service reliable and accessible? | Influences long-term cost |
| Lifecycle Planning | What is the expected replacement timeline? | Impacts total ownership cost |
This framework ensures that cost comparison extends beyond price and reflects operational realities.
Common Misconceptions Distort Equipment Cost Comparisons
Several misconceptions lead to inaccurate cost evaluations across veterinary hospitals. These misconceptions often result in suboptimal purchasing decisions.
Common misunderstandings include:
- Assuming lower purchase price equates to lower total cost
- Overestimating utilization without supporting data
- Ignoring maintenance and service variability
- Treating all equipment categories as financially equivalent
- Underestimating the impact of workflow integration
Accurate comparison requires disciplined evaluation across all cost dimensions.
FAQ: Veterinary Equipment Cost Comparison
How do corporate veterinary groups achieve lower equipment pricing?
Why do independent hospitals often pay more for equipment?
What is the most important factor in determining equipment cost efficiency?
Does financing method significantly impact total cost?
How do vendors influence long-term equipment cost?
Is standardization always more cost-effective than customization?
How should hospitals evaluate whether to invest in new equipment?
Equipment Cost Strategy Reflects Broader Operational Philosophy
Veterinary equipment cost comparison ultimately reflects how an organization balances efficiency, flexibility, and clinical alignment. Corporate systems optimize for scale and consistency, while independent hospitals optimize for precision and adaptability. Future cost strategies will increasingly depend on data integration, lifecycle planning, and alignment between technology capability and clinical demand.